I-Team In-Depth
Pediatric Psychiatric Cases Continue Climbing, Swamping ERs
|
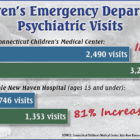
The state’s efforts to direct children in mental health crisis away from emergency rooms, to other services, have fallen short, with major hospitals reporting staggering increases in patient visits since 2013: Up 32 percent at Connecticut Children’s Medical Center, and 81 percent at Yale New Haven Hospital. The children’s hospital (CCMC) reported nearly 3,300 visits last year – 275 a month, on average — with the average length of stay increasing to 15 hours from less than 12 in 2013. “I wish I could say we had made a lot of progress, but we haven’t,” said Dr. Steve Rogers, medical director of the emergency department’s (ED’s) behavioral health unit. “Unfortunately, I think it’s only going to keep trending this way.”
Similarly, Yale saw ED visits by children ages 15 and younger rise from fewer than 750 in 2013 to more than 1,350 in 2016 — and the numbers are running even higher this year, said Dr. Claudia Moreno, medical director for psychiatric emergencies in Yale’s children’s emergency department. At times, she said, all ED beds are full, and children wait on hallway gurneys.