Dr. Erin Hofstatter, a young research scientist and breast cancer specialist at Yale’s Smilow Cancer Hospital, often prescribes tamoxifen, raloxifene and similar drugs to her patients. The drugs “reduce your risk (of cancer recurring) by half … but they come with baggage,” she tells her patients, “hot flashes, night sweats, leg cramps, small risk of uterine cancer, small risk of blood clots, small risk of stroke, you have to get your liver tested.”
Hofstatter’s unease with standard treatments for breast cancer has spurred her to seek alternative, safer ways to treat breast cancer. To this end, she has begun a study of black cohosh, in the pill form of an herb from the buttercup family, used for thousands of years by Native Americans to treat menopausal symptoms.
“There’s data to suggest that [black cohosh] is protective,” she said, “both in breast cancer survivors and potentially preventive in women who’ve never had breast cancer, based on a few large observational trials.”
Just as practices like acupuncture and meditation – once considered, at best, nontraditional are now widely used to help patients cope with the side-effects of cancer treatments and other illnesses, natural products – foods (blueberries, walnuts, soy), herbs like black cohosh and plant-based anti-oxidants like capsaicin (which makes hot peppers hot) have become accepted subjects for research.

Jenifer Frank Photo
Dr. Erin Hofstatter is studying black cohosh.
But far from simply embracing these practices or foods, scientists now apply rigorous scientific methods to what are considered non-traditional medications to determine just how effective – or ineffective — they are. A similar scientific focus is being directed at exercise, diet, and meditation. Research is also going on into something called energy healing.
“I think that when we think about therapies, whether for breast cancer or anything else, we do need to think outside of the box and evaluate things that we may not have been open to evaluating in the past,” said Dr. Anees Chagpar, director of The Breast Center – Smilow Cancer Hospital at Yale-New Haven. “Because there are natural therapies that may be very useful and helpful.”
“[T]here is a paucity of scientific evidence and research to back up these complementary and alternative approaches. And so I think that anything that we can do to help shore up the knowledge that we have about their utility is a good thing,” she said.
Alternative Medicine’s Integration
Once marginalized by the medical establishment, alternative medicine has now become part of the establishment. The National Center for Complementary and Alternative Medicine (NCCAM) is one of the 27 institutes and centers that comprise the country’s premier research institution, the National Institutes of Health (NIH).
NIH data show that funding for NCCAM research projects has climbed from $54.3 million in 2000, to $97.6 million in 2014 – an 80 percent increase. Among the grantees in 2014 is Yale University, which received nearly $1 million for four research projects into complementary and alternative medicine – including one study, with the Dana-Farber Cancer Institute and the Susan G. Komen Breast Cancer Foundation – that is testing “mindfulness meditation” for children suffering from fibromyalgia or chronic pain.
In addition, the American Board of Integrative Medicine plans to give its first accreditation test in November. The exam will include questions on “Mind-Body Medicine and Spirituality” and “Whole Medical Systems” (such as homeopathy, Traditional Chinese Medicine and the ancient Indian system, Ayurveda), as well as on nutrition, dietary supplements and “Lifestyle, Prevention and Health Promotion.”
The Consortium of Academic Health Centers for Integrative Medicine, which began in 1999 as a small group trying to draw attention to and expand the use of integrative medicine, has grown into an organization of 57 medical centers, many connected to some of the country’s most prestigious medical schools and health organizations. The consortium includes the integrative medicine programs at Yale and UConn’s schools of medicine, and the Integrative Medicine Center at Griffin Hospital in Derby, which collaborates with Yale.
Alternative medicine’s evolution is at least partially fueled by public enthusiasm. A widely quoted 2007 survey, by the National Center for Health Statistics, shows that in 2006, Americans spent $33.9 billion out-of-pocket on alternative medicine. Some health professionals say this shows the widespread dissatisfaction with the traditional health system.
“Our current health care system is not sustainable. It’s not working, it’s too expensive, and people are really not that healthy,” said Dr. Mary P. Guerrera, a family practice physician at St. Francis Hospital and Medical Center in Hartford who also directs the integrative medicine program in the Department of Family Medicine at the University of Connecticut School of Medicine.
Given the popularity of alternative treatments, “It’s important for future physicians and health professionals to learn about [them],” she said. Guerrera said she’s seen “a huge bump” in the number of fourth-year medical students taking the elective course she teaches, “Integrative/Complementary and Alternative Medicine.”
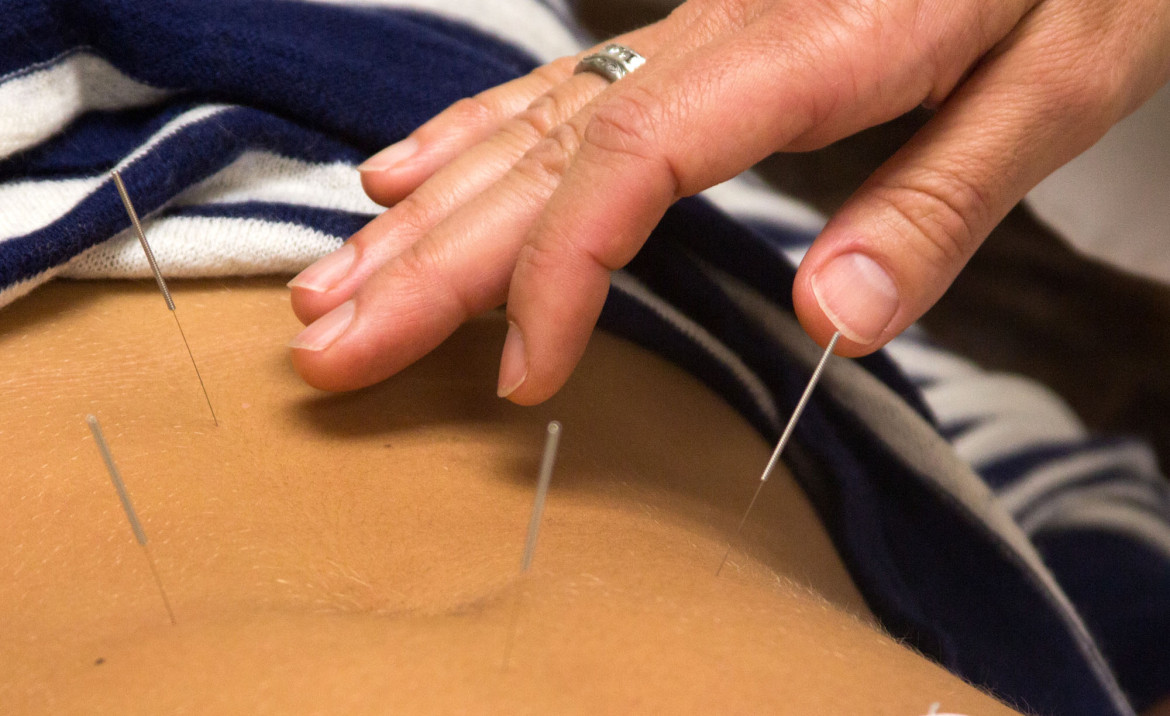
Deborah Pacik, a second year UConn medical student and a longtime licensed acupuncturist, has treated cancer patients for pain, nausea and depression. “Patients have felt more energy, less nausea, more appetite, less dry mouth, and calmer and clearer with acupuncture,” she said.

Tony Bacewicz Photo
Deborah Pacik, a licensed acupuncturist, treats cancer patients.
But alternative medicine continues to have its critics. They can be found on such websites as Quackwatch.com and The Skeptic’s Dictionary. Dr. Steven Novella, a researcher and assistant professor of neurology at Yale School of Medicine, founded the take-no-prisoners website Science-Based Medicine, of which he is editor. On Sept. 29, the site’s managing editor, Dr. David Gorski, a surgical oncologist, posted his latest attack on alternative medicine: “Quackademia Update: The Cleveland Clinic, George Washington University, and the continued infiltration of quackery into medical academia.”
Rigorous Investigations
A growing number of researchers are ignoring that skepticism by using scientific methods to measure and quantify the efficacy of unconventional treatments.
The NCCAM’s website is packed with warnings about not replacing traditional medical care with an alternative measure, and with understated dismissals of some claims from the marketplace. (On the acai berry, sold in fruit juice and as supplement: “There is no definitive evidence that acai has any special health benefits.”)
Chagpar, at Yale, summarized the attitude and motivation of many researchers: “There really needs to be further rigor to look at [complementary and alternative] therapies with the degree of scientific inquiry that we put routine drugs through.”
Hot Peppers
In his 27 years as a surgeon and researcher at the Yale School of Medicine, Dr. John Geibel’s research has focused on the lower digestive system. But these days, he’s also excited about the anti-carcinogenic power of capsaicin on breast cancers. Capsaicin – capsicum is any plant from the nightshade family — is the substance that gives hot peppers their heat, and, perhaps counter-intuitively, it has been identified as having some value as a pain reliever.
Geibel, vice chairman of the Department of Surgery at Yale, noted that genetic screening has been effective in determining whether some women will get breast cancer. “But even if you come in and perform the mastectomy, it’s difficult to impossible to remove every single [cancer] cell,” he said.
Earlier studies have shown capsaicin’s ability “to slow down or even stop the machinery of [cell] division,” he said, pointing to one in which capsaicin stopped the growth of prostate colonic tumors in a dish. What if, he posited, after a surgeon has removed a malignant tumor from a breast, the doctor can “coat the underlying tissue area with a capsaicin-based preparation to prevent any residual cells” from reproducing?
Geibel said he initially tested capsaicin on breast cancer cells in a culture to determine the dose and the best way to deliver it. “The next phase is to now take some tissue from an individual,” he said.
“It’s a relatively simple natural product,” he said. The goal of using products like capsaicin is “to have a destructive effect on the tumor, rather than a destructive effect on the individual.”
Energy Healing
With training in molecular and cellular biology, Dr. Gloria Gronowicz, a professor at the UConn Health Center, has long been looking into the effects of energy healing on tumor growth and metastasis, working most recently with a breast cancer model in mice.

Tony Bacewicz Photo
Energy healing on tumor growth is an area of study for Dr. Gloria Gronowicz.
Energy medicine, which includes Reiki, qigong and a practice named “Therapeutic Touch,” actually involves no direct touching of a patient or an object being studied. Rather, practitioners work with what they say is the energy emitted from their hands, which they call biofields.
A paper published in May by Gronowicz and others, in the Journal of Complementary and Alternative Medicine, said that Therapeutic Touch had prevented cancer cells in a breast cancer model from spreading, though it had not shrunk the size of the primary tumor.
“Let us use everything to help patients,” Gronowicz said of the growth in research into alternative treatments.
Black Cohosh
Hofstatter, the Yale researcher, first heard of black cohosh from the gynecologic oncologist who runs Yale’s Sexuality, Intimacy and Menopause Clinic. The oncologist asked if Hofstatter would approve of giving Remifemin – a pill form of black cohosh – to one of the young doctor’s patients.
“I was actually fearful of black cohosh to begin with,” Hofstatter said. “It basically is a plant-based estrogen, and so many times, breast cancers can be fed by estrogen.” But she found ofstattetwo 2007 clinical trials that showed black cohosh acting as a protective agent in breast cancer development.
The more she researched, “the more I realized, ‘Oh my gosh, I may have just struck a pot of gold!’ ” she said. “Not only does it not appear to significantly increase the risk of breast cancer, but actually there’s data to suggest it’s protective, both in breast cancer survivors and potentially preventive in women who’ve never had breast cancer.”

Black cohosh
Her study, funded by Yale through the American Cancer Association, focuses on women diagnosed with DCIS, ductal carcinoma in situ — a common, noninvasive cancer that can develop into an invasive disease.
The trial takes advantage of the time between a diagnosis of DCIS and the surgery, generally two to four weeks. Right after diagnosis, the patient will take Remifemin twice daily until her surgery. Hofstatter thenH will compare the pre-surgery DCIS cells and those in the tissue removed during surgery to see if the number of DCIS cells has dropped.
“What I liked about the study is that I felt the risk to the patient was minimal” — because she was going to have surgery anyway – “and that it would provide good information regardless of what we showed.”
Hofstatter, who received her grant in 2011, is still recruiting subjects for the study, and hopes to have her roster filled by 2015.
And she is clear-eyed about her hopes for black cohosh. “I have no idea if it works,” she said.
“The reason we’re doing the trial is because I do not know if it helps. For all I know, it could be bad — that’s the thing about research.”
Join C-HIT Tuesday, Oct. 21, starting at 5:30 p.m., at Gateway Community College, New Haven, for a community forum on the latest inroads and challenges in breast cancer detection, research and treatment, while showing your support for in-depth journalism. For information and to register click here.