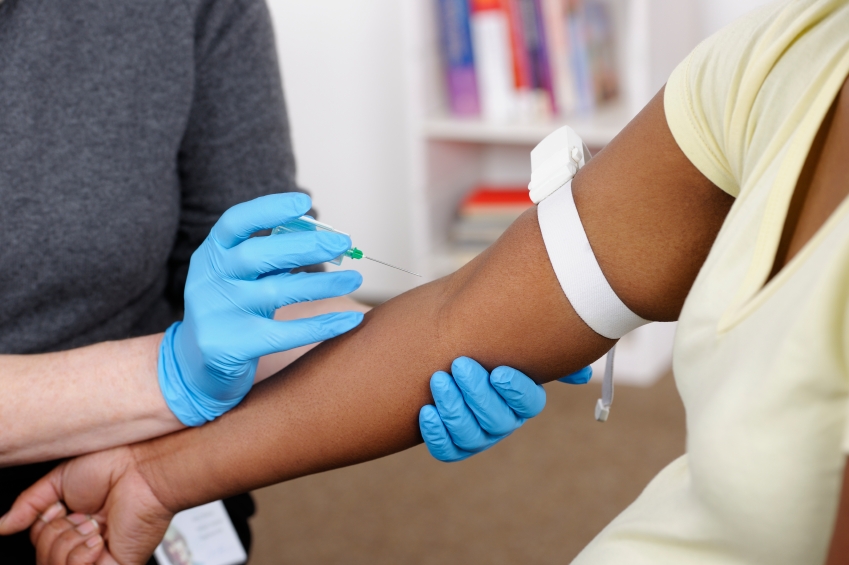
A simple blood test is transforming the world of prenatal screening, offering women a risk-free way to learn about fetal abnormalities early in pregnancy.
Already, the new test has drastically reduced the demand for amniocentesis, an invasive procedure that diagnoses chromosomal disorders in mid-pregnancy and occasionally causes miscarriage. The blood test, which became available in late 2011, can analyze DNA to predict Down Syndrome and a few other genetic diseases as early as nine weeks in pregnancy, says Dr. Daniel Gottschall, medical director of Women’s Health Connecticut, a group practice with 80 offices around the state.
“It’s almost like science fiction to see how they can do this with such a high level of accuracy,” says Leslie Ciarleglio, a genetics counselor at Hartford Hospital, where the number of amniocentesis procedures plummeted by more than 70 percent in just two years — from 112 in 2011 to 32 in 2013. “It’s far more accurate than any screening test we’ve had before.”
The test, which experts consider one of the most important clinical tools to emerge so far from the genomics revolution, can alleviate fear and suffering for pregnant women worried about birth defects. But the medical advance also raises disturbing questions about the future of screening — and whether the quest for the perfect baby could go too far.
Currently, most women who get the blood tests are carrying high-risk pregnancies. They are either older than 35 or have had ultrasounds that indicate potential problems. But some testing companies now offer the genetic analysis to all pregnant women, giving many access to information they never planned to seek out.
 If the blood test is negative, there’s more than a 99 percent chance that the fetus doesn’t have the most common chromosomal abnormalities, says Gottschall, who is vice chairman of obstetrics and gynecology at St. Vincent’s Medical Center, and in private practice in Bridgeport.But if the test is positive, that doesn’t necessarily mean that the fetus has medical problems. So, genetic counselors urge women with positive test results to follow up with amniocentesis, which can conclusively diagnose the presence of genetic disease.
If the blood test is negative, there’s more than a 99 percent chance that the fetus doesn’t have the most common chromosomal abnormalities, says Gottschall, who is vice chairman of obstetrics and gynecology at St. Vincent’s Medical Center, and in private practice in Bridgeport.But if the test is positive, that doesn’t necessarily mean that the fetus has medical problems. So, genetic counselors urge women with positive test results to follow up with amniocentesis, which can conclusively diagnose the presence of genetic disease.
“Screening is not definitive,” says Jennifer Hoskovec, president of the National Society of Genetic Counselors. Although she says the blood test is a “fantastic technology” that allows families to get reliable information early in pregnancy, “it’s not a replacement for a diagnostic test.”
Nationally, more than 90 percent of women who discover they are carrying a baby with a chromosome disorder decide to get abortions, studies show.
The novel-screening test grew out of a series of discoveries that date back to the late 1990s. In 1997, a Hong Kong chemist detected fetal cells circulating in pregnant women’s blood, describing his finding as learning that the engine of a car was not just under its hood. For years, health care providers predicted that the stunning revelation would quickly trigger major medical changes. But it took more than a decade for scientists to figure out the best way to apply this new knowledge.
Eventually, they realized they should analyze only fetal cells that were falling apart, focusing on the DNA spilling out of cells into the mother’s bloodstream, experts say. The DNA, or deoxyribonucleic acid, makes up chromosomes, which scientists can examine to figure out whether the fetus carries a severe genetic disorder.
Companies developed what came to be known as the cell-free DNA blood test, which analyzes the DNA that has leached out of fetal cells. The blood tests can screen for three kinds of chromosome abnormalities: Down syndrome, which affects 1 in 1,000 babies born each year, as well as the less common Edwards and Patau syndromes that also cause severe birth defects.
“It’s truly a profound change,” says Peter Benn, who directs the University of Connecticut’s diagnostic human genetics laboratory and consults for one of four U.S. companies that analyze the cell-free DNA blood tests. It’s transforming pregnancy, he says, “taking away a lot of the fear and anxiety.”
Until the advent of cell-free DNA, pregnant women concerned about genetic problems typically opted for one of two invasive tests with miscarriage risks. Chorionic villus sampling, usually conducted during 10 and 12 weeks of pregnancy, involves placing a catheter in the cervix and a 1 in 100 chance of miscarriage. Amniocentesis, by contrast, offers more comprehensive and definitive information about fetal health and has smaller odds of miscarriage – between 1 in 300 or 1 in 500. Typically performed after 15 weeks of pregnancy, it involves inserting a needle in the uterus.
Since the cell-free DNA test became available in November 2011, demand has exploded; with more than a half-million tests nationally being ordered through 2013, says Benn, who consults for Natera, a California-based genetics testing company. And as scientists devise ways to advance the technology, it’s clear that the test may soon be recommended to many more women, not just those carrying high risk pregnancies.
Already, the American College of Medical Genetics and Genomics says the test should be offered to all pregnant women. Many medical societies continue to support restrictions, since most of the research on the technology involved women at high risk of having children with birth defects.
But that research is rapidly changing. Just last February, the New England Journal of Medicine published a study showing that the fetal DNA test was ten times better at predicting Down syndrome in all pregnant women than the standard blood and ultrasound tests. Natera, meanwhile, announced in February that its non-invasive screening tests can now detect DNA imperfections called microdeletions that cause serious medical conditions. One such imperfection, which is just as common as cystic fibrosis, can cause heart defects, deformed palates and immune problems.

today.uconn.edu
Peter Benn at UConn.
As the science rushes forward, ethical quandaries are emerging – especially fears that the tests could lead to a spike in abortion. The cell-free DNA test could soon be used to screen all pregnancies, vastly expanding the number of women who learn about fetal abnormalities, bioethicists argue. Only 5 percent of pregnancies are now screened with amniocentesis.
With the new tests, potential medical problems could be identified in the first trimester, when abortion is easier to get and more women are willing to consider it. And it’s possible that the tests could eventually predict potential health problems that a child might suffer from as an adult, such as developing breast cancer at age 50 – raising even more complicated ethical issues.
Already, the Chinese and Indian governments are banning testing companies from divulging the gender of the fetus to expectant families – out of fear the information could lead to a spate of abortions of females.
In the U.S., health care providers are currently focused on more mundane concerns, such as tracking testing companies’ policies on evaluating low-risk women and figuring out how much – if anything — insurers will pay for the pricey assessments. The test can cost as much as $2,800 – more than ten times more than the typical first trimester screening, Ciarleglio says. If insurers balk, the testing companies are sometimes willing to subsidize the bulk of the expense, she says.
Aside from costs, there’s still confusion about what the tests can actually determine. Many women continue to falsely believe that the test can completely replace amniocentesis, Ciarleglio says. While the blood test can screen for the major chromosome disorders, amniocentesis can diagnose more potential birth defects. The difference occurs, in part, because the blood test examines cells that were in the fetus’ placenta, while amniocentesis looks at cells – often discarded skin cells – that were floating in the amniotic fluid.
For healthy pregnant women over 35, it’s rarely an important distinction. If their blood test is negative and a subsequent ultrasound shows no problems, then they can skip amniocentesis, Ciarleglio says.
Clearly, many women in Connecticut are now skipping these tests. At Women’s Health Connecticut, the number of amniocenteses dropped by half in the past two years, Gottschall says. Similarly, Yale- New Haven Hospital saw a 45 percent decrease during that time, with amniocenteses sinking from 265 to 146 between 2011 and 2013. At Bridgeport Hospital, the number of amniocenteses dropped from 29 in 2011 to 12 in 2013.
Some women may not be candidates for the new blood tests, such as obese women, who typically have so little cell-free DNA in their bloodstream that results would be less accurate. On average, about 10 percent of a pregnant women’s cell-free DNA comes from her fetus.
Only a few women have received inaccurate results from Hartford Hospital, which conducts the screening in Hartford as well as satellite offices in Meriden and New Britain. Two women of the more than 700 tested were notified that their child might have a chromosomal problem, but a follow-up amniocentesis showed the fetus had no genetic defects, Ciarleglio says.
Mostly, women are thrilled that the new procedures could reduce the need for invasive procedures, she says.
“It’s counterintuitive for a pregnant woman to let someone put a needle in her uterus,” she says. “Most women want to avoid that, if they can.”