Connecticut was among 41 states nationwide to earn a failing grade from health advocates for lacking public information about the quality of care provided by doctors.
“Consumers should be able to find out if their local primary care physician is delivering good quality care without having to go through hoops,” said Francois de Brantes, executive director of the Health Care Incentives Improvement Institute in Newtown, which published the report. “Connecticut has no public reporting of physician quality.”
Only two states, Minnesota and Washington, received an ‘A.’ California received a ‘C’ and the remaining states earned a ‘D’ or ‘F.’
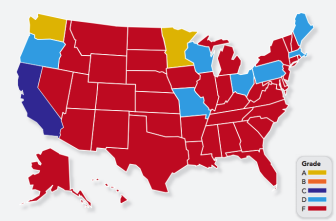
Only two states received an 'A' for public reporting of physician quality.
Mark Schaefer, the state’s new director of Healthcare Innovation, wasn’t surprised by the findings. “It’s widely recognized that consumers in the health care market don’t have accessible and reliable information about the cost of treatments across settings and the quality of providers at the clinical level,” he said. “Like most states, this is something Connecticut is working on.”
The “State Report Card on Transparency of Physician Quality Information” scored states on many factors, including the number of doctors rated, whether the ratings included information about clinical outcomes and consumer experiences, and how easy it was to access information online.
Having access to transparent information about provider quality and costs has become increasingly important as consumers facing higher insurance deductibles and out-of-pocket expenses try to make informed decisions when comparing physician networks and health plans.
In Connecticut, health experts expect the All-Payer Claims Database (APCD) currently under construction, and health care delivery and payment reforms to play important roles in establishing performance, quality and cost transparency. Last week’s announcement by the Connecticut Hospital Association that members take steps by March 1 to inform patients about facility fees if they receive care at hospital-owned medical offices was another step toward greater price transparency.
Assessing a provider’s performance poses special challenges because “often times quality is in the eye of the beholder,” said Matthew Katz, executive vice president and chief executive officer for the Connecticut State Medical Society, which represents more than 7,000 physicians. “What constitutes as quality for one insurer, provider or consumer may be completely different for another.”
Many of the current sources of physician performance data from the federal government, commercial insurers and non-profit organizations are often “inconsistent, incomplete, invalid and inaccurate,” offering only a “small snapshot” of a doctor’s entire practice, said Katz.
“You can’t just throw numbers out there without explaining the criteria used to determine quality and providing a road map for improvement,” he said. “Data presented in isolation doesn’t provide a true and accurate picture of the care being provided.”
A physician’s ranking, for example, may not reflect the limitations set by health plans. “How can you tell primary care physicians they’re going to be evaluated for quality but they can’t refer patients to all the specialists in their community,” said Katz.
Health care providers and consumer advocates also worry about the process used by commercial insurers to decide which doctors and facilities to include in provider networks. They cite United Healthcare’s recent decision to remove more than 2,000 Connecticut doctors from its Medicare Advantage network. Two Connecticut county medical associations have sued United Healthcare.
“Consumers need to know whether rankings are based on clinical outcomes, cost savings or both,” said Katz.
Keith Stover, lobbyist and spokesman for the Connecticut Association of Health Plans, did not respond to requests for comment.
Nationwide, states with passing grades on performance transparency had state-specific initiatives with insurers, providers and consumers to develop a universal system of identifying and recording data and defining quality, noted Katz. “The goal is to provide information that is actionable and accessible,” he said.
Changes underway nationally and statewide bode well for consumers. To start, Medicare officials plan to release data on physician quality collected by the federal government later this year, according to de Brantes.
A new state law requiring health care professionals who provide direct patient care at facilities to wear identification badges with their credentials is a positive step toward transparency, said Katz. “Truth in advertising is part of quality,” he said. “Consumers need to understand a provider’s scope of practice to know if he or she can provide the services they truly need.”
Performance transparency is a major element of the Connecticut Healthcare Innovation Plan submitted to federal officials in December, said Schafer, who is leading the state initiative. The plan calls for the creation of a common performance scorecard for providers beginning with primary care physicians. Providers also would be accountable for the quality and cost of care and, in some cases, benefit from savings.
Information collected for the APCD under construction by Access Health CT, the insurance marketplace created by reform, will shed light on quality and performance, as well. Access Health received a federal grant to implement the large-scale database that collects medical, dental and pharmacy claims from commercial insurers and public insurers such as Medicare and Medicaid. Consumers will have access to the data in a free web-based portal.
“All of these multiple sources will provide consumers with a more reliable reflection of true performance,” said Schaefer.
To read the report by the Health Care Incentives Improvement Institute click here.