Disparities
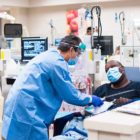
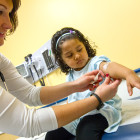
Education, Across All Demographics, Is An Effective Prescription To Combat Diabetes
|
Since Nydia Rodriguez met Wanda Santiago about a year ago, the New London resident has lost 20 pounds and gotten her Type 2 diabetes under control. That’s because Santiago, Lawrence + Memorial Hospital’s bilingual diabetes educator, has taught Rodriguez, a former nurse from Puerto Rico, about portion control, sugar substitutes and how to cut back on bread and pasta. Santiago, who was also a nurse in Puerto Rico, has even connected Rodriguez with food banks that offer fresh fruit and vegetables. “I talk to her almost every day,” Rodriguez, 64, said in Spanish, with her daughter Yolanda Mejias translating. “If I need anything, I’ll call her.”
Diabetes is the seventh leading cause of death in the U.S. and the main cause of kidney failure, lower-limb amputations and adult blindness.