COVID-19 Risks Could Speed Transitions To At-Home Dialysis
|
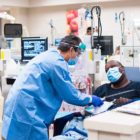
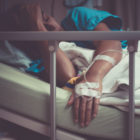
The COVID-19 pandemic will likely result in a “huge paradigm shift” toward in-home dialysis treatments in the future, experts predict. Home “is the safest place for them to be,” said Dr. Holly Kramer, president of the National Kidney Foundation and a practicing nephrologist. In times like this, immunocompromised individuals are at increased risk of becoming ill. Roughly 85% of dialysis patients get their treatments in centers—often three days a week, and typically for several hours at a time—where other dialysis patients also are being treated, she said. Before the COVID-19 outbreak, nephrologists nationwide were urging a growing number of patients to consider at-home care, she said, and the pandemic “will push things much, much faster” in that direction.