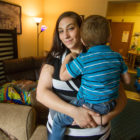DCF’s New Strategy: Treating Children And Families In Their Own Homes
|
Last May, Samantha Collins’ drug use, legal problems and dealings with the Connecticut Department of Children and Families forced her to strike a bargain with the agency. In return for allowing social workers to come into her home three times a week to help her stay off drugs, improve her parenting and learn the practical skills needed to function as an adult, DCF would not remove her children. The 26-year-old Somers mother of 2- and 7-year-old boys entered Family-Based Recovery, a program created 10 years ago by DCF, the agency better known, perhaps, for separating families than working to keep them together. Family-Based Recovery, or FBR, is an example of DCF’s dramatic reversal in philosophy and practices, after years of a policy approach based largely on removing children thought to be at risk and placing them in congregate care facilities. “‘Pull and ask later,’” said Kristina Stevens, a former DCF social worker who is now administrator of the agency’s Clinical and Community Consultation and Support Division, which includes a fast-growing array of in-home treatment programs.
As recently as 2011, nearly 1,500 children and youths were separated from their families and were living in 54 group homes and other treatment centers in and out of Connecticut.