Coronavirus
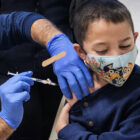
UPDATED: Coronavirus In Connecticut
|
The state’s weekly COVID summary: 1,027,729 residents have tested positive for COVID-19, with 3,827 testing positive over the last 7 days; the 7-day positivity rate is 15.56%, the state Department of Public Health (DPH) reported. The state reported 16,026,603 PCR/NAAT tests, with 24,598 residents testing positive over the last 7 days. Hospitalizations total 714. The state reported 37 deaths, bringing the death total to 11,770. DPH is releasing weekly COVID reports on Thursdays.