I-Team In-Depth
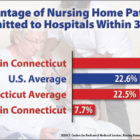
New Strain On State Nursing Homes: Keep Patients Out Of Hospitals
|
At the Fresh River Healthcare nursing home in East Windsor, the chance that a short-stay patient will end up back in the hospital within 30 days of arriving at the facility is less than eight percent. Meanwhile, 12 miles away at the Greensprings Healthcare and Rehabilitation nursing home in East Hartford, more than a third of patients who came from hospitals will be readmitted in 30 days. The wide swing in nursing home patients’ re-hospitalization rates has a lot to do with the condition patients are in when they are discharged from inpatient stays, as well as the planning that goes into the transition to other care. The federal government has been penalizing hospitals since 2012 for high rates of patients returning within 30 days of discharge. But now, nursing homes (or skilled nursing facilities) also are being held accountable for hospital readmissions.