I-Team In-Depth
Filling The Primary Care Gap: Nurse Practitioners
|
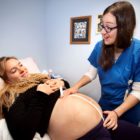
Alison McGrory-Watson, a private cook who lives in Deep River, had serious medical problems, including Hepatitis C and post-traumatic stress disorder (PTSD), when she was assigned Nichole Mitchell as her primary care provider at Community Health Center Inc. (CHC) in Middletown. McCrory-Watson was uninsured, and Mitchell went to great lengths to get financial assistance for two new drugs aimed at addressing her medical problems. As a result, McGrory-Watson is now Hep C-free, and she hopes a drug she’s taking for PTSD will quell the lingering effects of being gang-raped as a teenager and witnessing a brutal stabbing as an adult.
There’s something about Mitchell that might surprise you. She’s not a doctor; she’s a nurse. A nurse practitioner (NP), to be precise. But McGrory-Watson insists that the care Mitchell provides is every bit as good as she would get from a physician.