Thirteen-year-old Estrella Roman and her mother have made the 30-minute walk to Rogers Park Middle School in Danbury several times during the pandemic, even when the school has been closed for in-person learning. That’s because the school’s on-site health center is where Estrella, who emigrated with her family from Ecuador in 2019, receives routine vaccinations, wellness care, and treatment for headaches, among other health services.
Estrella’s mother, Katherine, who doesn’t speak English, said through Estrella that she’s “very grateful” for the teachers who told her that Estrella could still receive care there even when schools were closed. She praised the school nurse as patient and Spanish-speaking and said she would not have known where to seek care if not for the school-based health center.
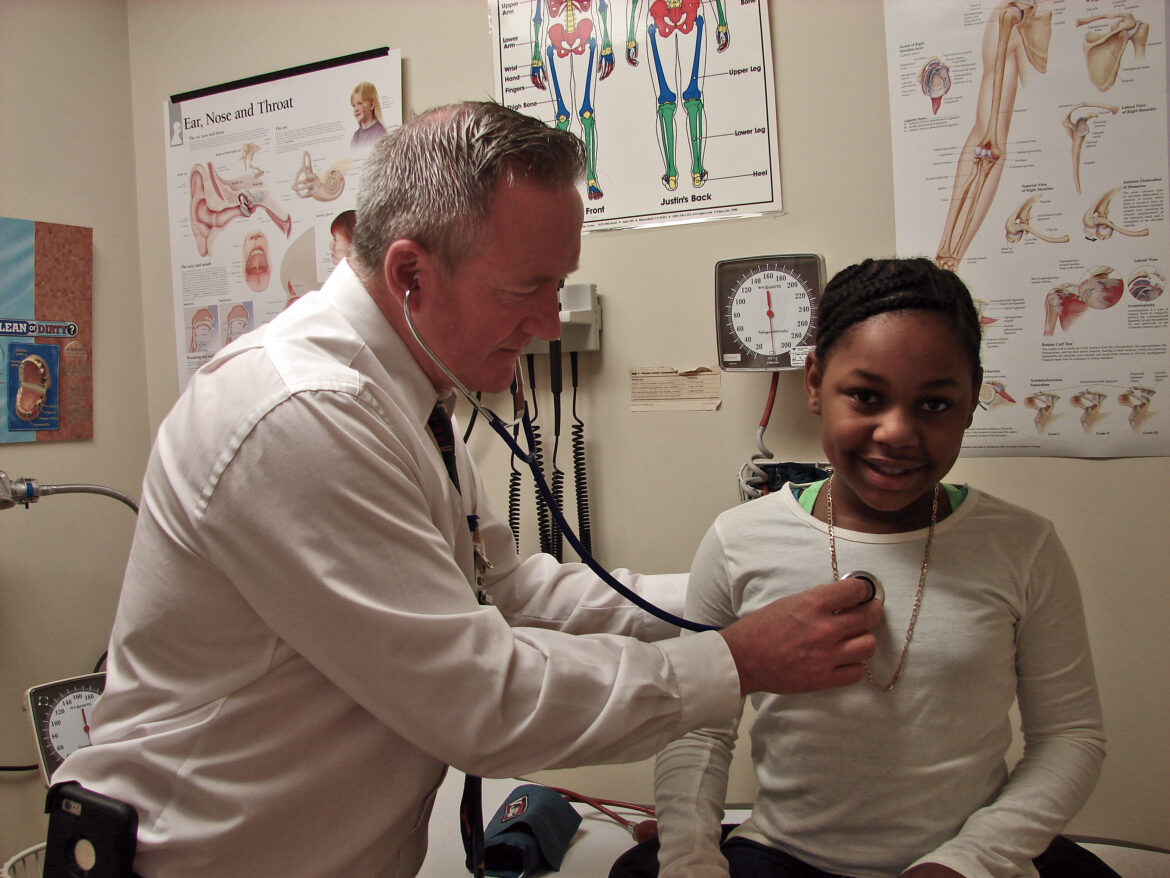
During their three decades in operation, Connecticut’s school-based health centers – defined by the state as fully-licensed primary care facilities — have become a critical health care delivery option, especially for children who have limited access to regular medical care.
Of the 92 school health programs funded by the state Department of Public Health, located in 27 communities throughout the state, 80 are designated “school-based health centers” and provide full health care services, including diagnosis and treatment of acute injuries or illnesses; managing chronic diseases; physical exams; immunizations; prescribing and dispensing medication; reproductive health; laboratory testing; crisis intervention; individual, group and family counseling; oral health; referral for specialty care; and links to community providers. The other 12 “expanded school health programs” offer limited services.
According to the DPH, 20,216 students made 62,159 medical visits to a school-based health center in 2018-2019, an average of 3.1 visits per student. A total of 4,589 students made 60,697 mental/behavioral health visits, an average of 13.2 visits per student, while 3,814 students made 9,557 dental visits, an average of 2.5 visits per student.
Since last March, as Connecticut public schools have fluctuated between closed, open and somewhere in-between, the health centers have worked hard to continue providing services uninterrupted.
“During COVID, all the school-based health centers have continued to offer medical and behavioral health care through a mix of on-site and telehealth visits,” said Laurie Collins, executive director of the Connecticut Association of School Based Health Centers.
Telemedicine has enabled New Haven Public Schools’ 16 health centers to continue providing mental health visits at pre-pandemic levels, according to Sue Peters, director of the district’s school-based health centers and dental clinics. In a typical year, she says, the centers would welcome nearly 7,000 visits for students’ medical, behavioral and dental needs, or about 60 percent of the student body.
She said she can’t yet calculate how many students utilized the centers in 2020 because “there’s too many factors to consider,” she said.
The change hasn’t been easy, say health center personnel. A lack of daily access to students has had a negative impact on drop-in visits and follow-up appointments. Dental care, which makes up a large part of many of the centers’ treatment services, has been on hold during the pandemic due to the threat of COVID-19 transmission. But creativity and flexibility have enabled health center personnel to continue performing certain vital health care services for students and, in some instances, adding new COVID-19-related resources.
Nurse practitioner Jolene Henion describes the health center at Rogers Park Middle School, where she works, as typically busy, providing a mix of physicals, vaccines, and acute care to students. Rogers Park turned to remote learning in March. At that time, the school’s health center transitioned to telehealth. But in June, when the center got the go-ahead to return to the building part-time, staff began to set up regular on-site drive-through vaccination clinics for children.
The need was pressing. The state didn’t waive routine immunization requirements during the pandemic, and the drive-through clinics present a safe option for families who don’t feel comfortable going into a doctor’s office during the pandemic. The clinics also serve families new to the area. In recent months, Danbury has experienced an influx of immigrants, mainly from Central and South America, whose immunization schedules differ from those in the U.S.
“They don’t qualify for health insurance, but we can at least get them registered for school,” said Henion, who notes that proof of up-to-date vaccinations is a prerequisite for school enrollment.
Health center personnel also work to keep students up to date on annual physicals. Henion calls families to remind them if their children are due for one. When students come in—the center has been open four days a week for wellness visits since August 2020—many show signs of pandemic-related weariness. “I’m having kids complain about back pain. They’re sitting all day, and not necessarily at a chair. Many are in bed, hunched over a computer,” Henion said. “They’re sedentary. They’ve all gained weight.”
Mental health issues are also skyrocketing.
“I’m seeing a huge uptick in anxiety and depression,” said Clare Gelissen, a licensed therapist who works at the health center on the campus of Danbury’s Henry Abbott Technical High School. Currently, the school operates in a hybrid format, with daily in-person student attendance at 25%. But despite the barely inhabited campus, Gelissen says she’s been busier than ever. “We’re definitely seeing an increase in kids,” she said.
The addition of telemedicine has made it easy for Gelissen to stay busy; the effects of the pandemic have made it necessary. “These kids are so isolated from their primary source of social interaction,” she said.
The state’s health centers also have taken on new roles during the pandemic. Many are involved in COVID-19 testing, according to Collins. Since December, Rogers Park Middle School has offered COVID-19 testing clinics multiple times each week, staffed by health center personnel. Any member of the school community experiencing symptoms can attend the clinic free of charge. But despite this and other ways health centers have remained relevant during the pandemic, it hasn’t been without downsides.

Sue Peters
New Haven’s Peters notes that typically their centers’ follow-up care is close to 100%. Now, she says, “It’s a struggle to get students to come in.” This, she says, despite the current safety protocols, whereby appointments are spaced out and few people are in the buildings at one time.
Henion agrees. “We’re so used to having such great access to kids. Normally, I can track them down any time,” she said. She’s particularly concerned about uninsured students who aren’t connected to a primary care provider in their community.
“They’re the ones I worry about,” Henion said. “I’m desperate to get the kids back.”
Yes! Indeed there’s a great need to make CT K-12 schools more healthy. In June 2019, Dr. Velandy Manohar (pediatric psychiatrist) & I submitted a testimonial to CT Commission on Educational Technology about School-Based Health Centers. This was also submitted to the State Office of Health Strategy initiative on ‘Health Enhanced Community’.
Public Testimony – SB Chatterjee: Education Technology and School-Based Health Centers [PDF file]
https://portal.ct.gov/DAS/CTEdTech/Commission-for-Educational-Technology/Meetings/June-3-2019
Yes – there’s a great need to make CT K-12 schools more healthy. In June 2019, Dr. Velandy Manohar (pediatric psychiatrist) & I submitted a testimonial to CT Commission on Educational Technology about School-Based Health Centers. This was also submitted to the State Office of Health Strategy initiative on ‘Health Enhanced Community’.