Reported cases of tuberculosis jumped 17 percent in Connecticut from 2014 to 2015, mirroring a national and global trend and prompting federal officials to ask primary care providers to be on the alert for at-risk patients.
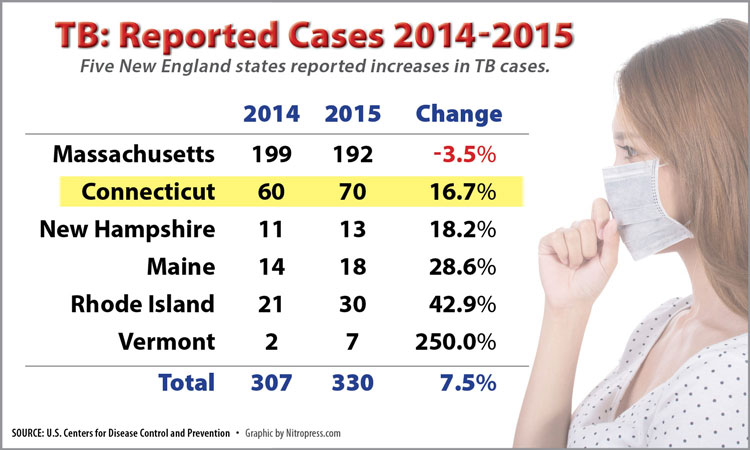
The state Department of Public Health (DPH) said 70 people, in 29 towns, were reported with active TB, the contagious form of the disease, in 2015, compared with 60 the year before. About 80 percent of Connecticut patients were foreign-born, many from Asian countries.
Nationally, TB cases totaled 9,563 last year, an increase of 157 over 2014. It was the first jump in cases after more than two decades of annual declines, the U.S. Centers for Disease Control and Prevention (CDC) reported. New England had one of the largest regional upswings, federal figures show, with 330 reported cases, a 7.5 percent increase.
Connecticut and national health officials are unclear on what’s behind the uptick and said more studies are needed. Drug-resistant strains have become a challenge, but that’s largely a problem overseas at this point, they said. About two-thirds of the cases nationally in 2015 were foreign born, the CDC said.
 Dr. Lynn Sosa, deputy chief epidemiologist at the DPH and head of its tuberculosis control program, said that most of the foreign-born residents had been in Connecticut for years, indicating they may have had the latent form of the disease. “Most did not get here last year,” she said.
Dr. Lynn Sosa, deputy chief epidemiologist at the DPH and head of its tuberculosis control program, said that most of the foreign-born residents had been in Connecticut for years, indicating they may have had the latent form of the disease. “Most did not get here last year,” she said.
Sosa was quick to say that she wants to see 2016’s numbers before considering this a trend, rather than a one-year spike. “Are we at a place we haven’t seen before? I don’t know,” she said.
Dr. James Mazo, medical director for occupational health at St. Francis Hospital and Medical Center in Hartford, said tuberculosis is “a disease we tend to think is pretty much nonexistent. But it’s still out there.”
Yale New Haven Hospital consistently treats five to 15 patients a year with active TB, said Dr. Richard A. Martinello, medical director of infection prevention. Officials of other Connecticut hospitals say they treat roughly similar numbers.
For many years, tuberculosis was the leading cause of death in the U.S. Spread by airborne bacteria; it most often strikes the lungs, but can affect any part of the body.
Although its numbers have been cut dramatically since the mid-20th century with the advent of multidrug therapies, TB resurged with the HIV/AIDS epidemic, which offered a new supply of hosts with weakened immune systems.
Most TB patients in the U.S. were born in Mexico, the Philippines, India, Vietnam and China. In Connecticut, the three countries of origin with five or more cases in 2015 were India, the Philippines and Ecuador, the DPH said.
The Stamford Advocate reported in February that 31 people were tested after coming into contact with someone with active TB in the city’s Westhill High School community. Dr. Henry Yoon, medical adviser for the Stamford health department, said he was unaware of anyone who was tested contracting the disease.
Dr. Michael Parry, an infectious disease specialist with Stamford Hospital, said many of the eight to 10 patients a year the hospital sees come from Central America and the Caribbean, as well as India. The patients are “infected during childhood, they immigrate here, and during adulthood, the TB reactivates,” he said. “It has smoldered and then escapes [the] immune system’s control.”
He compared latent tuberculosis to shingles, a far more common condition, which is caused by the reactivation of the virus that causes chickenpox.
Symptoms typical of active tuberculosis include a persistent cough, fever, chills and unintentional weight loss. People with latent TB – the World Health Organization and CDC estimate this group as a third of the world’s population – show no symptoms of the disease, and they are not contagious.
Since the uptick was announced, the CDC has ramped up prevention efforts, targeting people with a high risk of latent infection — about 13 million people, or about 4 percent of the U.S. population. Without treatment, one in 10 of them will develop active tuberculosis, the agency said.
In addition to people from countries with a high prevalence of the disease – comprising much of the developing world – HIV patients or others with weakened immune systems are considered high risk, as are people who live or have lived in certain congregate settings, such as homeless shelters and long-term care facilities.
For the first time, the CDC says the public health system is no longer the only crucial player in prevention.
“[W]e need help from [primary care providers] to encourage at-risk patients to get tested, and if needed, start and complete treatment,” Dr. Philip LoBue, director of the CDC’s Division of Tuberculosis Elimination, said in a September statement.
Health experts say it’s easier and much less expensive to treat latent TB than full-blown tuberculosis. Treating active TB can take six to nine months — if there are no complications — and it’s extremely labor-intensive, requiring medical personnel to watch patients take each dose of medicine.
In addition to “deputizing” primary care providers and emphasizing treatment of latent infections, the CDC is also updating its 10-year-old guidelines on preventing transmission to health care workers who treat TB or HIV.
Two hospitals in Connecticut have reported testing large groups of employees recently after they may have been exposed to contagious patients, according to the 2016 UConn Health Center report on occupational diseases for the state Workers’ Compensation Commission.
About 80 workers at William W. Backus Hospital in Norwich, in both 2013 and 2014, had to be tested, said Tim Morse, professor emeritus at the health center and the report’s coauthor.
In 2014, St. Francis Hospital tested about 250 employees who may have been exposed to two patients with TB.
None of the hospitals’ employees contracted either an active or latent infection, doctors with each institution said.
Mazo, St. Francis’ medical director for occupational health, said that in the 2014 incident, “Unfortunately, it was three to four days before [the two patients] could be diagnosed, and [they] had gone to multiple departments…We then backtracked and notified colleagues” who may have had contact, he said.
Dr. Jack Ross, chief of infectious disease at Hartford HealthCare, said, “It’s important to remember that TB presents with a myriad of nonspecific symptoms.
“Depending on location, potential TB exposures occur yearly in many hospitals,” Ross said. “This is despite the most rigorous screening and attempts to predict which patients pose a risk.”
Tuberculosis is one of humanity’s oldest killers — traces have been found in the bones and tissues of Egyptian mummies — and it remains one of the world’s most deadly infectious diseases.
For information on TB and who should be tested click here.
Nice overview. TB is a disease that requires constant vigilance by providers and public health officials lest it raises it’s head again.