Federal investigators have found that Medicare officials rarely enforce rules for private insurance plans intended to make sure beneficiaries will be able to see a doctor when they need care.
It’s a problem many Connecticut seniors know too well. In 2013, UnitedHealthcare, the nation’s largest health insurance company, dropped hundreds of health care providers from its Connecticut Medicare Advantage plan, including 1,200 doctors at the Yale Medical Group and Yale-New Haven Hospital. Medicare Advantage beneficiaries scrambled to find new insurance or new doctors while the Fairfield and Hartford counties medical associations went to court to try to stop the terminations.
The report by the Government Accountability Office, the investigative arm of Congress, said that Medicare did not check provider networks to ensure that doctors were available to beneficiaries and cited Connecticut as a “case study” in what can go wrong.
The GAO report shows that Medicare “was not verifying network adequacy. That’s their job and they abdicated that responsibility,” said U.S. Rep. Rosa DeLauro, D-New Haven, who requested the investigation along with other members of the Connecticut congressional delegation.
“The recommendations in the report will close many of the loopholes that health insurers use to unfairly reduce the size of its physician networks and, in the process, drop those patients who cost the insurers more money to cover,” said Mark Thompson, executive director of Fairfield County Medical Association.”
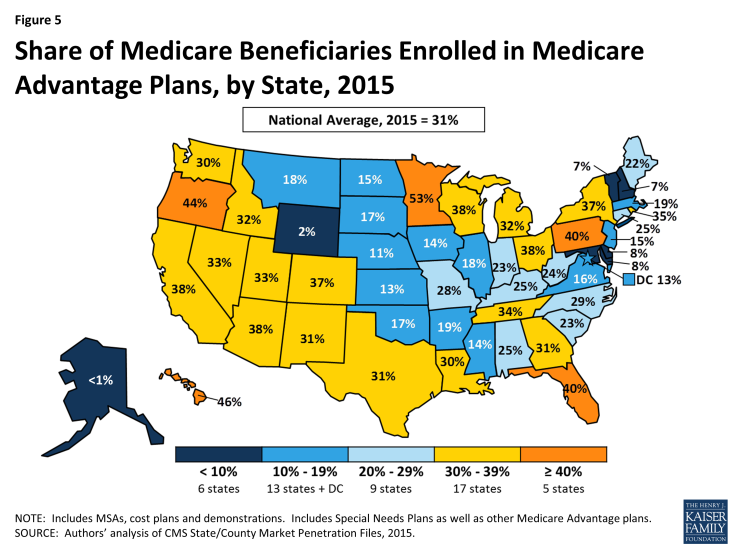
Medicare Advantage coverage is sold by insurance companies as an alternative to traditional Medicare, and may offer better benefits and lower prices in some parts of the country. Nearly 17 million older Americans have signed up for these policies, including 157,000 in Connecticut. Enrollment for next year begins Oct. 15.
Medicare Advantage beneficiaries are restricted to a network of providers. If their provider leaves, they cannot change plans during the year. Two years ago, UnitedHealthcare cut its network shortly before open enrollment began so seniors had an opportunity to make changes in coverage for the coming year.
But many have few choices if they want to stay in Medicare Advantage. Nearly 90 percent of Connecticut seniors in the program are enrolled in plans from three companies: UnitedHealthcare, EmblemHealth and Aetna, according to an analysis by the Kaiser Family Foundation.
The U. S. Centers for Medicare and Medicaid Services (CMS), which oversees Medicare Advantage, requires the plans to have doctors in sufficient numbers and specialties who are near enough—in distance and travel time—so that seniors can reach them. Specific requirements vary to according to geographic area and population.
 But the GAO found that CMS checked the provider networks of less than 1 percent of the plans since 2013—serving just 2 percent of Medicare Advantage members—and only when the plans expanded to a new county. For the rest, CMS relies on data from insurers to confirm that the networks meet the requirements.
But the GAO found that CMS checked the provider networks of less than 1 percent of the plans since 2013—serving just 2 percent of Medicare Advantage members—and only when the plans expanded to a new county. For the rest, CMS relies on data from insurers to confirm that the networks meet the requirements.
When new provider networks do not comply, the GAO found that CMS invited plans to request an exemption, and nearly all were granted.
“The thing that jumped out at us is how little the networks are reviewed,” said James Cosgrove, director of health care. “And when exceptions are granted, they are not revisited—both of those were very surprising to us.”
The provider network information insurers submit to CMS contains the same flawed details “as in provider directories, which have been shown to be inaccurate in a number of government and private studies,” the GAO also found.
In a written response included in the report, U.S. Health and Human Services Assistant Secretary Jim Esquea told Cosgrove the government is “committed to ensuring Medicare beneficiaries receive high quality health care” and agrees with several GAO recommendations for improvements.
For example, CMS now agrees that notices to beneficiaries who are losing their doctors should contain specific standard information, and improvements are needed in the computer system used for network adequacy reviews. The agency also said it would require next year’s provider directories to indicate whether providers accept new patients.
In the Connecticut case study, the GAO said that UnitedHealthcare told CMS about the provider cuts in July 2013, but the agency didn’t scrutinize the impact on beneficiaries until October, after providers found that they would be cut and complained to CMS. Then CMS began weekly phone calls with UnitedHealthcare to monitor the situation.
Investigators also confirmed that UnitedHealthcare cut Medicare Advantage providers in 23 other states, more than twice the number elected officials and medical associations reported at the time.
“United was so irresponsible and I believe they thought they were going to get away with it,” said DeLauro, the senior Democrat on the House health subcommittee of the appropriations committee.
“This report tells us what many of us have longed suspected,” said U.S. Sen. Richard Blumenthal, D-Conn. “We must hold CMS accountable for their laziness and their appalling lack of scrutiny, which has endangered millions of seniors’ ability to access to health care.”
UnitedHealthcare spokesman Matt Burns did not respond to questions about specifics of the report, but said the company offers Medicare Advantage members “a broad choice of doctors.”
Burns said updating provider directories “remains an industry-wide concern” and the company is working with health care providers “to improve accuracy.”
The lawsuit filed by the medical associations of Fairfield and Hartford counties against UnitedHealthcare didn’t completely block the 2013 cuts but they did win a court decision that said the company could not drop an association member until the doctor had an opportunity to challenge the action before an independent arbitrator.
Thompson said the arbitration results are confidential but many doctors he knows who received termination notices are still in UnitedHealthcare’s Medicare Advantage network.
DeLauro said the best protection for seniors in Medicare Advantage is her proposed legislation, called the Medicare Advantage Participant Bill of Rights, which would prohibit insurers from terminating providers without cause except during the annual fall enrollment period.
The insurance industry has criticized the bill because it assumes that contracts between plans and providers span a full calendar year when in reality they are negotiated throughout the year.
DeLauro said the GAO report will attract additional bipartisan support for her legislation and has already succeeded in getting the response from CMS that lawmakers sought. “The GAO helps to elevate this issue,” she said. “There are a lot of ways to get to Rome.”