I-Team In-Depth
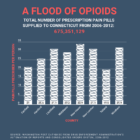
Calls To Rethink The War On Opioids
|
When three 13-year-old boys were sickened by the powerful synthetic opioid fentanyl at a Hartford middle school on Jan. 13, it was a shocking reminder of the human toll of the opioid crisis. One of the boys later died and a sweep of the school surfaced 40 small plastic bags of the drug. Later that same day, dozens of people spoke out against a proposal to locate a methadone clinic on a commercial street on the New Haven-Hamden border. During the ongoing battle with COVID-19, there seems to be less attention being paid to opioid addiction, advocates say.