Women's Health
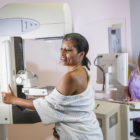
REACH Fund Begins Distributing Grants To Abortion Providers
|
The REACH Fund of Connecticut, a nonprofit organization dedicated to funding abortion care, has begun making grants to abortion providers. “People think that because abortion is legal here and Connecticut has a lot of wealthy areas that there isn’t a need, but there is,” said co-founder Jessica Puk. Medicaid covers abortion in Connecticut, but Puk says the fund will address a need among many marginalized groups, including undocumented women, low-income people who earn too much to be covered by Medicaid, and those who have private insurance with a high deductible or copay costs. “These are real people who need to access real health care and are hitting real barriers to it,” she said. Puk and three other women began organizing the fund in the summer of 2021.