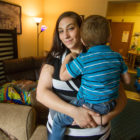I-Team In-Depth
Safety Net For Neglected Older Teens Can Be Difficult To Secure
|
Emily Kendricks has to eat soft foods, just like her grandfather. Although she’s only 18, she’s missing six teeth due to her parents’ dental neglect, advocates say. Her mother ignored her, excluded her from meals, and did not return urgent calls from Kendricks’ school guidance counselor, so Kendricks left home and moved in with a friend’s family. Despite efforts to bring Kendricks’ case to the attention of the state Department of Children and Families (DCF) by that counselor and her friend’s mother starting a few weeks after her 17th birthday, DCF did not take Kendricks into state care until shortly before her 18th birthday. “There was a long period of time where I couldn’t understand why DCF didn’t help,” Kendricks said.