Costs And Access Still Barriers To Health Care, Survey Finds
|
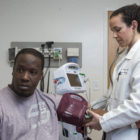
Iasiah Brown, 25, of New Haven, said he does not see a need for a primary care doctor for himself and his daughter, opting to visit clinics in the area instead of waiting up to two weeks for an appointment at a doctor’s office. Brown is among the 83 people who said they didn’t have a primary care doctor in response to a health-care usage survey by the Conn. Health I-Team and Southern Connecticut State University. The team surveyed 500 people and interviewed dozens statewide between January and March. About 83 percent of respondents said they had a primary care doctor, but the rate was lower for African American (78 percent) and Hispanic respondents (75 percent).