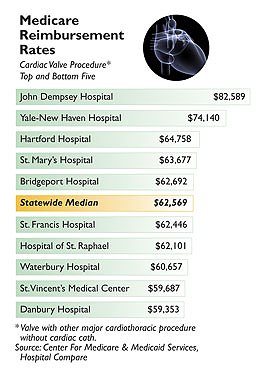
Each time John Dempsey Hospital performs a cardiac valve surgery, the hospital receives a median payment of $82,589 from Medicare – about $23,000 more than the median paid to Danbury Hospital for the same surgical procedure.
A pacemaker implant at Dempsey, part of the University of Connecticut, costs Medicare about $20,000—$2,200 more than Yale-New Haven, $3,500 more than Bridgeport Hospital and $6,300 more than the Hospital of Central Connecticut.
Federal reimbursements for surgical procedures swing widely among Connecticut hospitals, a C-HIT analysis of available Medicare data shows, with Dempsey receiving a higher rate than other hospitals for most procedures. Yale-New Haven, Bridgeport and Windham hospitals also were consistently among the top five in Medicare reimbursements, according to the data.
Experts say the variation in Medicare payments is due to a variety of factors, including the type of hospital (teaching or non-teaching), regional wages and salaries, the income mix and sickness of patients and the number of tests and services provided.
To read related story on consumers’ access to health care costs click here.
The amount Medicare pays to hospitals is set by the federal Centers for Medicare & Medicaid Services (CMS) in a payment structure that attempts to reflect ‘’the costs that reasonably efficient providers would incur’’ in providing care, according to CMS. In other words, the reimbursements serve as a rough gauge of the across-the-board expense of running a hospital, relative to others around it, experts say.
But there are other factors that push up costs at some hospitals, including a higher use of intensive-care beds, more visits by multiple doctors, and more tests such as MRIs and CT scans. Those treatment variables are attracting increasing scrutiny in Connecticut, as the state moves towards implementing health care reform and examines how hospitals are paid for services.
“In a system where we reward (by) fee for service—so that the more you provide, the more you get paid—we cannot have the type of health care reform we envision for our state,’’ said Jeannette DeJesus, the governor’s special advisor on health care reform. “If we’re going to do meaningful reform, we need to have payment reform.”
Hospital procedures and services do have set charges associated with each of them, but “that number is useless,’’ said Jonathan Skinner, an economist at Dartmouth College who closely studies health care cost data. That’s because hospitals rarely, if ever, receive the listed charge for a particular procedure. They receive a stream of payments from Medicare, Medicaid, government, military and private health plans, all of which may pay differently for the same procedure.
For consumers covered by private insurance, hospitals negotiate payments separately with each insurance company for procedures and services. The contracts are secret, so consumers lack the ability to compare cost and quality, and even hospitals are unable to compare themselves to one another. A single hospital may have as many as 600 different contracts with insurers. The system allows for wide differences in price on a host of medical procedures.
Though Medicare reimbursements are arrived at differently from the prices negotiated between hospitals and private insurers, they can vary just as widely. For a cardiac valve surgery, Yale-New Haven Hospital’s Medicare reimbursement was second highest after Dempsey, at $74,140, followed by Hartford Hospital at $64,758. The state median was $62,569.
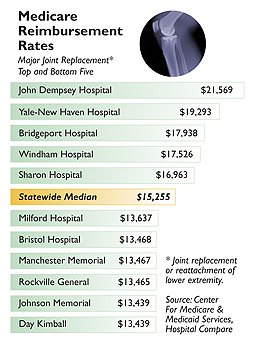
Medicare reimburses Dempsey for most surgeries at a higher rate than any other hospital in the state, including other teaching hospitals, the C-HIT analysis shows. Dempsey was paid a median amount of $21,569 for major joint-replacement surgery, for example, compared to a statewide median payment of $15,255. The lowest rate was paid to Day Kimball Hospital, at $13,343. For a major cardiovascular surgery, Medicare paid Dempsey a median of $54,655, compared to $36,966 for the Hospital of Central Connecticut.
Dempsey vs. Other Hospitals
Employee pay and fringe benefits, facility size, and the number of poor people treated contribute to Dempsey’s top reimbursement rate, said Cassandra Mitchell, associate vice president for reimbursement and financial systems at the University of Connecticut Health Center.
Unlike Yale-New Haven, Hartford and other teaching hospitals, Dempsey is staffed by state employees, whose fringe benefits are richer. Dempsey’s operating expense per patient day in fiscal 2010 was $5,458, according to financial data filed with the state. Yale-New Haven’s was $4,559, and Hartford’s was $4,180. Only Stamford Hospital, which is in the New York-metro area, had a higher expense per patient day, at $5,663.
A “good component’’ of the difference, Mitchell said, is Dempsey’s employee benefit packages.
Medicare also paid Dempsey more per patient because it’s a smaller teaching hospital than Yale-New Haven, Hartford, and others. Medicare reimburses teaching hospitals based on the ratio of medical residents to beds, and Dempsey’s ratio of 1.073 (meaning about one medical resident for each bed) is the highest in the state. The next highest is Yale-New Haven, at 0.6161, followed by Hartford, at 0.3803.
In addition, Medicare pays hospitals a greater amount if they have a “disproportionate share” of low-income patients.
“Medicare is saying, ‘We in the Medicare program recognize that if you take care of more poor folks, it will put an added burden on the overall institution,’ ” said Stephen Frayne, senior vice president for health policy at the Connecticut Hospital Association. ‘’ ‘So we’ll give you extra money, so that you’ll be more available to take care of Medicare patients, too.’ ”
The patient caseload on public assistance at Dempsey, located in suburban Farmington, is smaller than at urban hospitals, however. For example, state figures show that 18 percent of in-patients and 15 percent of outpatients at Dempsey are on Medicaid compared to 19 percent of in-patients and 35 percent of outpatients at Hartford; 22 percent of in-patients and 27 percent of outpatients at Yale-New Haven; and 28 percent of inpatients and 37 percent of outpatients at Bridgeport.
Mitchell said that Dempsey’s Medicare reimbursements were higher, in part, because low-income patients’ stays were longer in its neo-natal intensive care unit, and it treats patients with sickle-cell anemia and other blood disorders, which tend to require longer hospitalizations.
Though hospitals are reluctant to talk about it, there is another reason a facility’s Medicare payments can be higher than others, said Skinner: “It treats each patient more intensively.’’
Skinner and his colleagues have found in their studies that more-expensive hospitals show a higher use of intensive-care beds, more visits by multiple doctors and a greater use of home health care. In addition, the hospitals may order more tests, such as MRIs and CT scans.
“Aside from supplemental payments,” Skinner explained, “the only way hospitals can crank up reimbursements is by cranking up what they do. If you’re comparing two hospitals in similar areas with similar status . . . like, they’re both teaching hospitals, then they can still differ because of more readmissions and surgeries and other services.”
Consumer Access To Health Costs
Medicare accounts for only about one-fifth of the revenue that flows to hospitals, so its data alone cannot determine which hospitals are the most and least expensive. For Connecticut consumers, however, it’s the only available information that opens a window into hospital pricing.
Consumers in other states, including New Hampshire and Vermont, have the ability to review hospital costs because their states have developed “all-payer claims databases,” or APCDs, which collect an array of payment information. These databases allow consumers to compare costs of hospital procedures, and they help policy-makers and researchers to understand what’s driving health care costs, experts say. Connecticut has started an effort to build an APCD but it is in the planning stages.
Nationally, major changes to the hospital pricing system are underway. For instance, Medicare officials are working on ways to account for quality of care in reimbursing hospitals. Instead of fee-for-service medicine, which health reformers say offers financial incentives to providers to deliver more, and more costly, care, officials are looking at a system of global payments that would reward quality and efficiency.
Insurance companies are making similar efforts, said Joe Mundy, a spokesman for Cigna.
“There’s an increasing trend to identify areas of quality that can be measured and then reimburse hospitals appropriately, according to their quality and not simply their price,” Mundy said. That change will demand widely agreed-upon measures of quality.
Real change for consumers won’t come until they can readily compare prices, says James Stirling, president of Stirling Benefits in Milford, a benefits plan administrator.
“I think the status quo benefits from this lack of transparency,” said Stirling. “If you could figure out that a colonoscopy here, rather than there, will save money, then employers could build [insurance] plans that say, ‘We’ll pay 95 percent of the cost, and you’ll pay 5 percent.’ Then employees would have an incentive to shop around. You could say, ‘If you go to Yale, you’ll pay a $1,000 fee, but if you go to Milford, we’ll waive the out-of-pocket fee.’
“Until you have data that puts consumerism in the mix,” Stirling said, “we’ll be limited in what tools we can use to reduce hospital costs.”
The Fund For Investigative Journalism supported this work.
Under certain conditions, hospitals can have their “wage area” reclassified. Such is the case with Dempsey, thanks to its labor expenses. Its Disproportionate Share Hospital Patient Percent of 0.32312 is second only to Yale New Haven’s of 0.33474. The work done by Dartmouth’s Jonathan Skinner and his colleagues finds that, even after controlling for Medicare’s formulaic adjustments, more expensive hospitals cost Medicare more—because of such patterns-of-practice factors as more MRI use, more visits by physicians, etc.